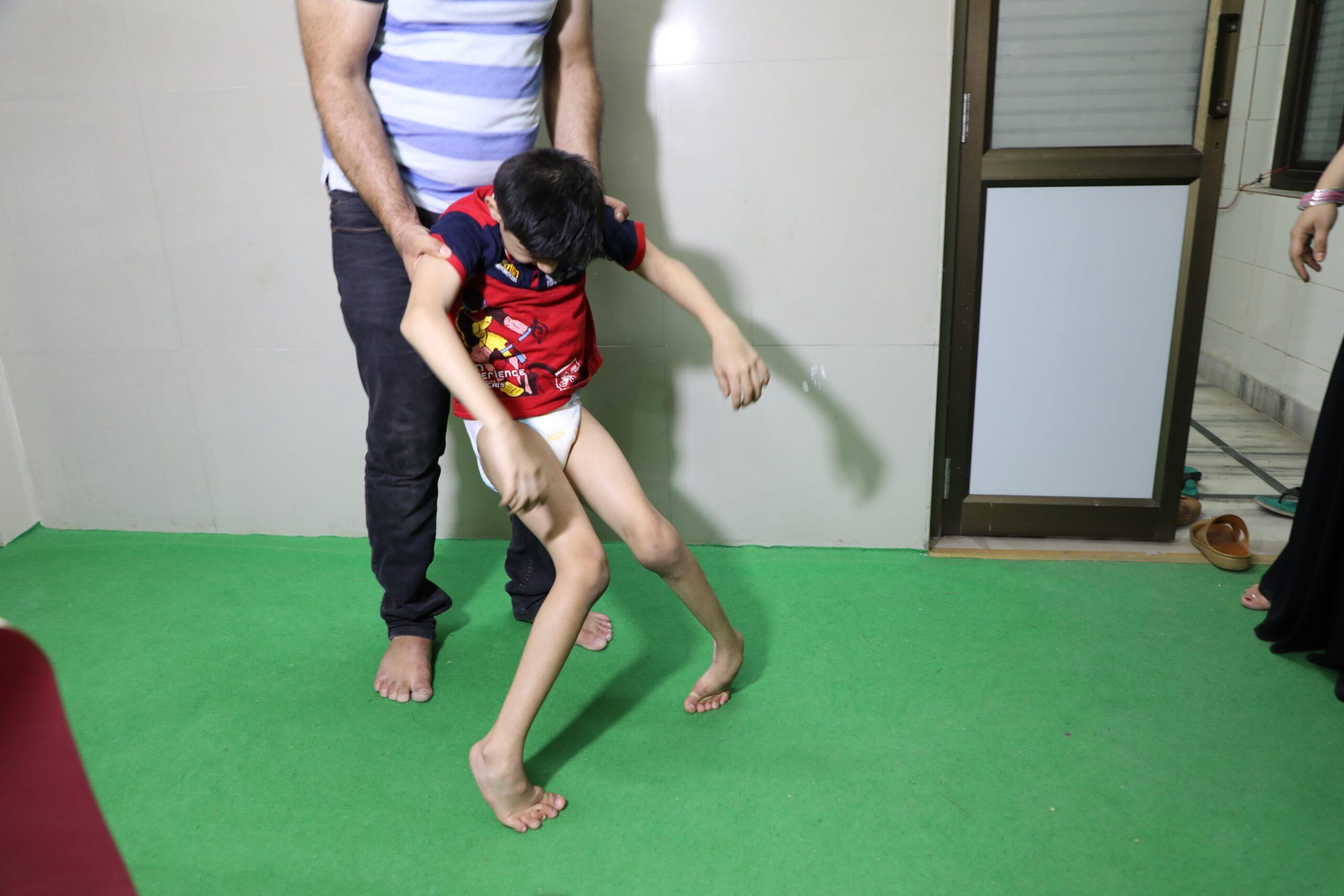
Cerebral palsy case studies
Cerebral palsy Treatment protocol in cerebral palsy affected individuals is decided on the basis of careful evaluation taking into consideration of clinical presentation (type), topography (extent of problem), age of individual, associated medical problem, GMFCS level, severity of disability etc. Every affected individual needs different set of treatment modality. Standard treatment protocol includes multimodal therapy program, brace, walking aid, botulinum toxin, surgery etc. All these techniques are being utilised in different combination based on the requirement of child. Advanced therapeutic modality is the primary modality of treatment in these children and this should be continued for long duration.
No one can decide exact treatment modality without detail evaluation. Treatment protocol given below is only a guideline but final decision has to be taken only after detailed evaluation of every individual child including static physical examination, gait analysis and lastly examination under anaesthesia. Treatment required in similar looking children can differ from guideline given below. The medical technology in cerebral palsy treatment is evolving and new researches are coming up frequently, so all this general information can change with new research guidelines in future.
There are multiple therapies available that help in cerebral palsy treatment. Therapy such as physical therapy, Occupational therapy, speech therapy, brace will help a lot in cerebral palsy treatment.
CP Specialized Doctors
CP Treatments & Therapy
%
Successful CP Treatment
Case Study Subjects
Cerebral Palsy Botulinum Toxin(Botox)
Sometime early age kids affected with spastic cerebral palsy don't show much improvement even with good...
Ataxic Cerebral Palsy By Dr. J. K. Jain
Ataxic cerebral palsy occurs because of the lesion in the cerebellum. The child has a very shaky &...
What Is The Best Treatment For Mild Cerebral Palsy?
What Is The Best Treatment For Mild Cerebral Palsy? Mild cerebral palsy means the child can walk and do his...
Case Study On Hemiplegic Spastic Cerebral Palsy
Hemiplegic spastic cerebral palsy typically affects the upper & lower limbs on one side. Children can...
Hand activity problem in cerebral palsy (HAND DEFORMITY)
Problem: Common problem in upper limb is pronation deformity, spasticity of finger & wrist flexor,...
Case Study On Diplegic Spastic Cerebral Palsy
Diplegic spastic cerebral palsy affects both lower limbs . It also features some functional problems...
Scissor Gait – CP Case Study
A scissoring gait is characterized by the knees & thighs pressed together or crossing each other while...
Jump Knee Gait / Toe Walking
Equines gait (Toe Walking) is the commonest deformity in cerebral palsy. In hemiplegic both soleus &...
In Toeing By. Dr. J. K. Jain
Problem:most of the time this intoeing occur because of increased femoral anteversion but some time they can...
Make a Difference
Support Trishla Foundation's Life-Changing Work for Children with Cerebral Palsy!
Together, we can break barriers and empower children with cerebral palsy. With your generous contribution, Trishla Foundation can continue its vital work in providing therapies, education, and support to these incredible children. Help us create a brighter future by donating today!